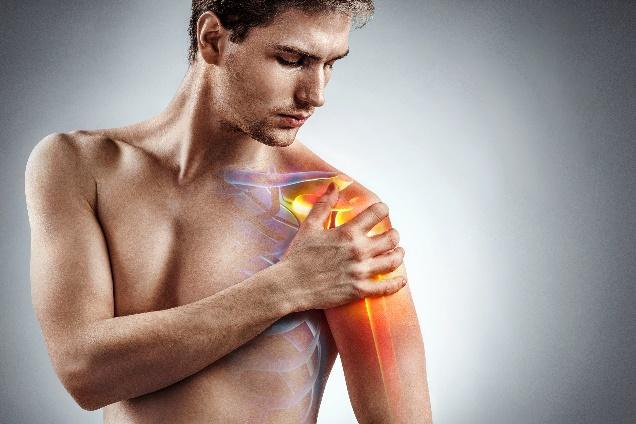
The brachial plexus is a network of peripheral nerves that relay information between the brain and the upper extremities. The bundle of nerves begins at the spinal cord near the neck and crosses the upper chest and armpit, traveling down the arms. There is a brachial plexus on each side of the body.
Dr. Jason Ko, a highly respected board-certified plastic and reconstructive surgeon, specializes in treating injuries impacting the brachial plexus and peripheral nerves to restore function to the shoulders, arms, and hands. If you have suffered a brachial plexus or peripheral nerve injury that affects your movement and sensation and causes you pain, Dr. Ko encourages you to consult with him promptly. Time is of the essence when treating these problems (ideally within six months of the injury); the earlier you seek intervention, the better the chances are that you will recover function in the affected areas.
Symptoms of Brachial Plexus Injuries
Brachial plexus injuries occur when the nerves are stretched, compressed, or torn away from the spinal cord. This can occur during accidents or traumas where the arm is forcefully pulled or stretched. Common causes of brachial plexus injuries include motorcycle or car accidents, sports accidents, or traumatic falls. Gunshot or penetrating (i.e., knife) wounds can also damage or cut the brachial plexus.
Some brachial plexus injuries occur during the birthing process as a complication of shoulder dystocia (i.e., difficulty delivering the baby’s shoulders after the head has been delivered); however, Dr. Ko focuses primarily on brachial plexus injuries in adults.
When the nerves of the brachial plexus become injured, it stops signals to and from the brain. This results in paralysis and weakness in the upper extremities. It can also cause chronic, debilitating pain, a burning sensation or numbness in the shoulders, arms and hands.
When consulting Dr. Ko about a suspected injury to the brachial plexus or peripheral nerves, he will perform a complete physical evaluation of your arm and shoulder’s range of motion and stability. He will inquire about any symptoms you experience, such as pain or numbness. Diagnostic tests such as MRIs, electromyogram (EMG) and ultrasounds may be performed to confirm or rule out a diagnosis.
Treatment of Injury
Some injuries to the brachial plexus recover with time and non-operative care, such as gentle stretching of the arm and shoulder, as well as physical or occupational therapy. The goal of therapy is to preserve or even extend range of motion and alleviate pain or discomfort. Exercises are designed to maintain the musculature and integrity of the shoulder joint.
If a brachial plexus injury is unlikely to improve on its own or with non-operative care, Dr. Ko may recommend surgical intervention. The appropriate surgical solution depends on individual factors such as the severity and complexity of the injury and the amount of time that has passed since the injury. Surgery repairs or reconstructs the nerves, sometimes requiring the use of nerve transfers or nerve grafts taken from another part of the body. Muscle transfer may also be incorporated into the surgical treatment of brachial plexus injuries to transplant a functioning muscle from another part of the body to the arm.
Contact Dr. Jason Ko
For more information about the diagnosis and treatment of brachial plexus injuries, please contact the practice of Dr. Jason Ko today.